BMI has guided clinical decisions for nearly 200 years. Body composition analysis has existed for decades. In 2026, the evidence is clear, but millions of patients are still being assessed with the wrong tool.
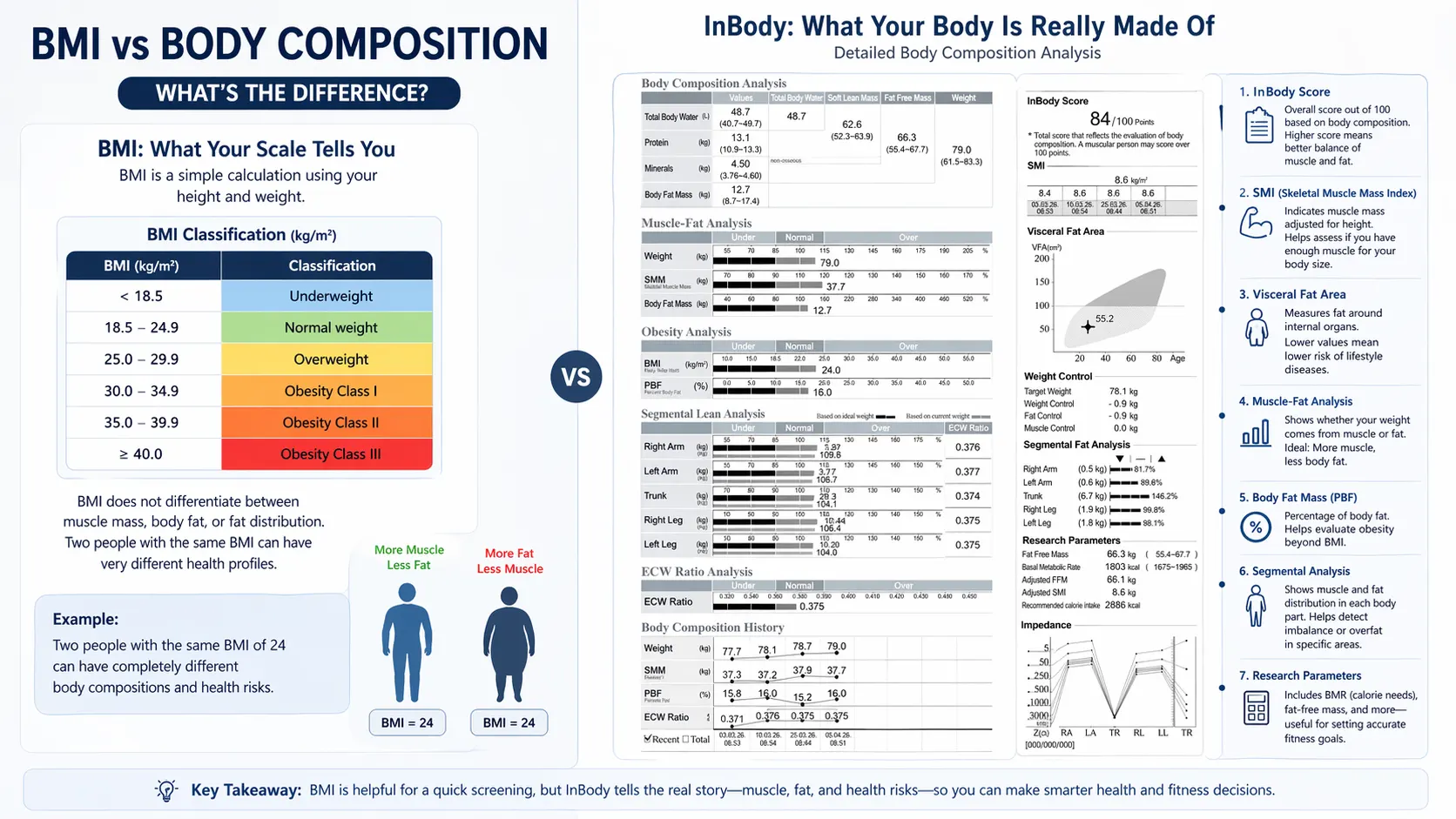
The BMI chart vs. the InBody body composition report: a direct comparison
Ask your doctor about your health, and there is a good chance they will reach for your BMI, a simple formula invented nearly 200 years ago. But in 2026, there is a better, faster, and more accurate option available in clinics across India. This article compares body composition analysis and BMI head-to-head and gives you the evidence to understand which one should be guiding your health decisions.
What is BMI, and what does it actually measure?
Body Mass Index was developed by Belgian mathematician Adolphe Quetelet in 1832. It was designed as a statistical tool for describing populations, not for diagnosing individual health. The formula divides a person’s weight in kilograms by their height in metres squared.
The result is a single number. That number is then placed into one of four categories: Underweight (below 18.5), Normal (18.5–24.9), Overweight (25–29.9), or Obese (30 and above). Based on that category, clinical decisions are made about cardiovascular risk, diabetes risk, surgical eligibility, and treatment thresholds.
The problem is not the maths. The problem is what BMI does not measure. It tells you the ratio of your weight to your height. It tells you nothing about what your weight is made of.
| In 1832, the BMI was invented for population statistics, not individual diagnosis | 1 in 4 Patients misclassified by BMI are wrongly labelled healthy or at risk | 0 params BMI measures zero parameters of actual body composition: fat, muscle, or visceral fat |
What is body composition analysis and what does it measure?
Body composition analysis measures the physical components that make up your body weight, separating fat mass, skeletal muscle mass, bone mineral content, and body water. Rather than asking “how much do you weigh?”, it asks the far more clinically useful question: “What is your weight made of?”
InBody’s Bioelectrical Impedance Analysis (BIA) technology sends safe, low-level electrical currents through the body. Because muscle and fat conduct electricity differently, the device calculates the exact mass of each tissue type in under 60 seconds, non-invasively, without radiation or blood draw.
- Skeletal Muscle Mass (SMM) is the total metabolically active muscle, the key driver of resting energy use and glucose disposal
- Body Fat Mass & Percentage: Total fat weight and its proportion of body weight, the true obesity indicator
- Visceral Fat Level: Organ fat rated 1–20. The strongest metabolic risk predictor, BMI, cannot detect
- Phase Angle: Cellular membrane integrity a marker of metabolic resilience and nutritional status
- Basal Metabolic Rate (BMR): Resting calorie requirement calculated precisely from fat-free mass, not total weight
- Segmental Lean Analysis: Muscle distribution in arms, legs, and trunk reveals imbalances that no overall metric can show
Head-to-head comparison: body composition vs BMI
| Clinical Criteria | BMI | Body Composition (InBody) |
|---|---|---|
| Measures body fat directly | No, estimates only | Yes, precise measurement |
| Measures skeletal muscle mass | No | Yes |
| Detects visceral fat | No | Yes |
| Identifies “skinny fat” (MONW) | No, classifies as healthy | Yes, body fat % reveals it |
| Accurate for athletes | No, misclassifies as overweight | Yes , low fat, high muscle confirmed |
| Accurate for Indian populations | Partially cut off too high | Yes, direct measurement bypasses cutoff issues |
| Guides nutrition plan (protein / calories) | No | Yes, BMR and FFM enable precise targets. |
| Tracks progress during weight loss | Partially, only the total weight | Yes, fat vs muscle changes are tracked separately |
| Detects cellular health (inflammation) | No | Yes, phase angle and ECW/TBW ratio |
| Cost and availability | Free, available anywhere | Requires the InBody device available at clinics |
| Time required | Instant calculation | Under 60 seconds |
| Clinical actionability | Low, four broad categories only | Highly specific, measurable parameters |
Body composition analysis wins on 10 of 12 criteria.
BMI retains only two advantages: It is free and requires no equipment. In every clinically meaningful category, fat measurement, muscle tracking, visceral fat detection, disease risk identification, nutrition guidance, and progress monitoring, body composition analysis is unambiguously superior. The question for 2026 is not which is more accurate. This is why BMI is still the primary tool.
Why BMI is especially inaccurate for Indian patients
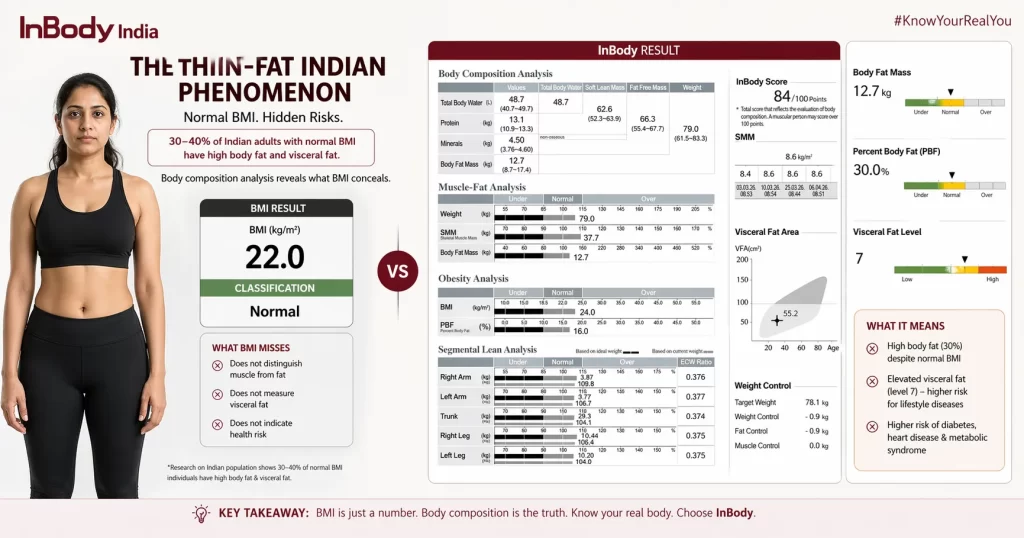
The BMI categories used worldwide were developed from data on largely Western, European populations. Indian bodies are physiologically different in ways that make these cutoffs clinically misleading.
- Indians carry more fat at lower BMI values: Landmark research by Yajnik and Yudkin (2004) documented the “thin-fat Indian” phenotype. Indian individuals have significantly higher body fat percentages at the same BMI compared to European populations. A BMI of 23 in an Indian patient may correspond to a body fat percentage that would be classified as overweight or obese by body composition standards.
- Indians have higher visceral fat at lower BMI: Studies consistently show that Indians accumulate more visceral fat, the metabolically dangerous fat around organs, relative to subcutaneous fat, compared to Western populations. This visceral fat drives insulin resistance and cardiovascular risk, yet it is completely invisible to BMI.
- Indians have lower muscle mass at the same BMI: Lower skeletal muscle mass is consistently reported in Indian populations compared to Western counterparts at equivalent BMI. This means the “healthy” weight label on the BMI scale masks a metabolically vulnerable body composition with less muscle to drive glucose disposal and metabolic rate.
- The WHO recommends lower BMI cutoffs for Asians: The World Health Organisation acknowledges that standard BMI cutoffs are inappropriate for Asian populations, recommending lower thresholds of 23 for overweight and 27.5 for obesity rather than 25 and 30. Even with these adjustments, BMI still cannot measure fat, muscle, or visceral fat directly. Body composition analysis bypasses the cutoff problem entirely.
The cost of using the wrong tool
An Indian patient with a BMI of 22.5 is classified as “Normal” and sent home without intervention. Their InBody scan shows 32% body fat, a visceral fat level of 12, and skeletal muscle mass below the healthy range, a clear MONW (Metabolically Obese Normal Weight) profile with significant cardiovascular and diabetes risk. BMI gave completely false reassurance. This scenario is not rare; it describes an estimated 30–40% of normal-weight Indians.
Four patient scenarios where BMI gives the wrong answer
| Patient Profile | BMI Says | InBody Reveals | Clinical Risk |
|---|---|---|---|
| Athletic individual with high muscle mass | Overweight / Obese | Low body fat, high SMM healthy | BMI triggers unnecessary intervention |
| Slim Indian adult, sedentary lifestyle | Normal | High body fat, low muscle, elevated visceral fat MONW | BMI misses significant metabolic risk |
| Elderly patient losing muscle with age | Normal or Underweight | Sarcopenia critically low SMM | BMI misses frailty and fall risk |
| Patient on GLP-1 therapy (semaglutide) | Improving weight falling | Fat AND muscle both falling poor quality loss | BMI gives false positive on therapy success |
When to use BMI, body composition, or both
BMI is not without utility. Understanding when each tool is appropriate helps clinicians get the most from both.
When BMI is appropriate
Large-scale population screening where individual precision is not required. Rapid initial triage in resource-limited settings where no body composition device is available. Epidemiological research comparing populations. Insurance and administrative classification, where a standard metric is required. Always as a starting point, never as a final clinical decision.
When body composition is essential
Individual clinical decision-making for metabolic disease risk. Managing diabetes, cardiovascular risk, or obesity, especially in Indian patients. Monitor weight loss or GLP-1 therapy to confirm fat is being lost, not muscle. Assessing elderly patients for sarcopenia. Designing personalised nutrition plans requiring accurate BMR and protein targets. Any patient for whom a treatment decision will be made based on the result.
When to use both together
BMI provides a fast, standardised baseline that can be recorded and compared across systems. Body composition analysis provides clinical depth. Using both together, recording BMI for administrative purposes and using InBody data for clinical decisions, gives practices the best of both worlds without losing the standardisation that BMI provides.
How body composition analysis is used in clinical practice

Diabetes & Endocrinology
Screen for MONW in normal-weight patients. Identify muscle loss in patients on GLP-1 therapies. Monitor insulin resistance patterns through visceral fat and muscle mass trends. Assess sarcopenic obesity as a high-risk condition in Indian diabetic populations that BMI cannot identify.
Cardiology & Preventive Medicine
Visceral fat level is a stronger cardiovascular risk predictor than BMI or waist circumference in Indian populations. Body composition analysis enables cardiac risk stratification beyond lipid panels and blood pressure, identifying hidden metabolic risk in clinically “normal” patients.
Nutrition & Weight Management
BMR calculated from fat-free mass enables accurate calorie prescription. Protein targets from fat-free mass are more precise than those based on total weight. Serial scans confirm whether weight loss is fat or muscle, the question that determines whether an intervention is working clinically or just cosmetically.
The 2026 clinical standard is what the evidence recommends
Medical bodies worldwide have been moving away from BMI as a standalone clinical metric for years. In 2023, the American Medical Association recommended against using BMI alone to assess health, citing its racial and gender biases. In India, the ICMR and clinical consensus groups on obesity and sarcopenia have highlighted the need for body composition assessment in Indian populations.
The evidence in 2026 supports a clear hierarchy:
- Body composition analysis should be the primary tool for individual clinical decisions about metabolic health, weight management, and disease risk
- BMI may be retained as a standardised screening tool and for administrative purposes, but never as the sole basis for clinical decisions
- For Indian populations specifically, body composition analysis is not optional; it is the only tool that accounts for the thin-fat Indian phenotype accurately
- Serial body composition scans, not serial BMI calculations, should be the standard for monitoring patients on weight management or pharmacotherapy programmes.
The Bottom Line
“BMI tells you if your weight is proportional to your height. Body composition analysis tells you whether you are metabolically healthy. In 2026, for individual patients, especially Indian patients, only one of those answers is clinically useful.”
Frequently asked questions
Q. Is body composition analysis more accurate than BMI?
Yes, for individual clinical assessment, body composition analysis is significantly more accurate than BMI. It directly measures fat mass, muscle mass, and visceral fat rather than estimating health from a weight-to-height ratio. BMI cannot distinguish between fat and muscle, cannot locate where fat is stored, and produces systematically inaccurate results in Indian, athletic, and elderly populations.
Q. Can someone have a normal BMI but unhealthy body composition?
Yes, this is called Metabolically Obese Normal Weight (MONW) or “skinny fat.” Research estimates 30–40% of Indians with normal BMI have body compositions characterised by high body fat, low muscle mass, and elevated visceral fat, all significant metabolic risk factors that BMI completely misses. Only body composition analysis can identify this condition.
Q. Why does BMI misclassify athletes as overweight?
Muscle is denser than fat. A given volume of muscle weighs more than the same volume of fat. Athletes with high muscle mass therefore weigh more than average for their height, pushing their BMI into the overweight or obese category despite having low body fat and excellent metabolic health. Body composition analysis immediately resolves this misclassification by measuring fat and muscle separately.
Q. Why is BMI less accurate for Indian patients?
BMI cutoffs were developed from data on Western European populations. Indians have a different body composition phenotype, storing more body fat and visceral fat at lower BMI values, and having lower muscle mass relative to body weight. The WHO recommends lower BMI cutoffs for Asian populations (overweight at 23, obese at 27.5), but even these adjusted cutoffs cannot directly measure fat or muscle. Body composition analysis bypasses this problem entirely by measuring tissues directly.
Q. How often should I get a body composition scan?
For general health monitoring, once or twice a year provides a useful baseline and trend. For patients actively managing weight, on pharmacotherapy (GLP-1 drugs, etc.), or undergoing nutritional intervention, every 4–6 weeks during the active phase allows timely identification of muscle loss and response to treatment. Always test under the same conditions, morning, fasted, before exercise for accurate comparisons.
Key takeaways
- BMI was never designed for individual diagnosis: Invented in 1832 for population statistics, BMI remains popular because it is free and fast, not because it is accurate. For individual clinical decisions, it is a blunt and often misleading tool.
- BMI cannot see fat, muscle, or visceral fat: These are the three metrics that define metabolic health risk. BMI measures none of them. Body composition analysis measures all of them in under 60 seconds.
- BMI is especially unreliable for Indian patients: The thin-fat Indian phenotype means 30–40% of normal-weight Indians have dangerous body compositions that BMI classifies as healthy. For Indian populations, body composition analysis is not a luxury; it is a clinical necessity.
- Body composition wins on 10 of 12 clinical criteria: BMI’s only genuine advantages are that it is free and requires no equipment. In every measure that matters clinically, fat detection, muscle tracking, visceral fat, disease risk, nutrition guidance, and body composition analysis are superior.
- The 2026 clinical standard is clear: Leading medical bodies worldwide are moving away from BMI as a standalone clinical tool. For individual patients, especially Indian patients, body composition analysis should be the primary metric guiding metabolic health decisions.
Give your patients the assessment they deserve
Move beyond BMI. InBody body composition analysis delivers the precise, actionable data that drives better clinical decisions in under 60 seconds, non-invasively, in any clinic setting across India.

Find an InBody Scanner Near You
Medical Disclaimer: This article is for informational and educational purposes only. It does not constitute medical advice, diagnosis, or treatment recommendations. All clinical decisions should be made by qualified healthcare providers based on individual patient assessment. InBody devices are not intended to diagnose, treat, or cure any medical condition.
References & further reading
- Yajnik CS, Yudkin JS — The Y-Y Paradox: The Thin-Fat Indian. Lancet, 2004;363(9403):163.
- WHO Expert Consultation — Appropriate body-mass index for Asian populations. Lancet, 2004;363(9403):157–163.
- American Medical Association — AMA Adopts New Policy Clarifying Role of BMI as a Measure in Medicine. June 2023.
- Bhardwaj S, et al. — Prevalence of Metabolic Syndrome Among Indians with Normal BMI. JAPI, 2013.
- Kalra S, et al. — Indian Consensus on Sarcopenia including T2DM Sarcopenic Obesity. Int J Gen Med. 2025;18:1731–1745.
- Prentice AM, Jebb SA — Beyond body mass index. Obesity Reviews, 2001;2(3):141–147.
- InBody — Body Composition Analysis in Metabolic Disease Management. Clinical White Paper, 2024.
- PMC 2021. Association of Body Composition with T2DM: InBody 770 retrospective chart review, n=2,404.