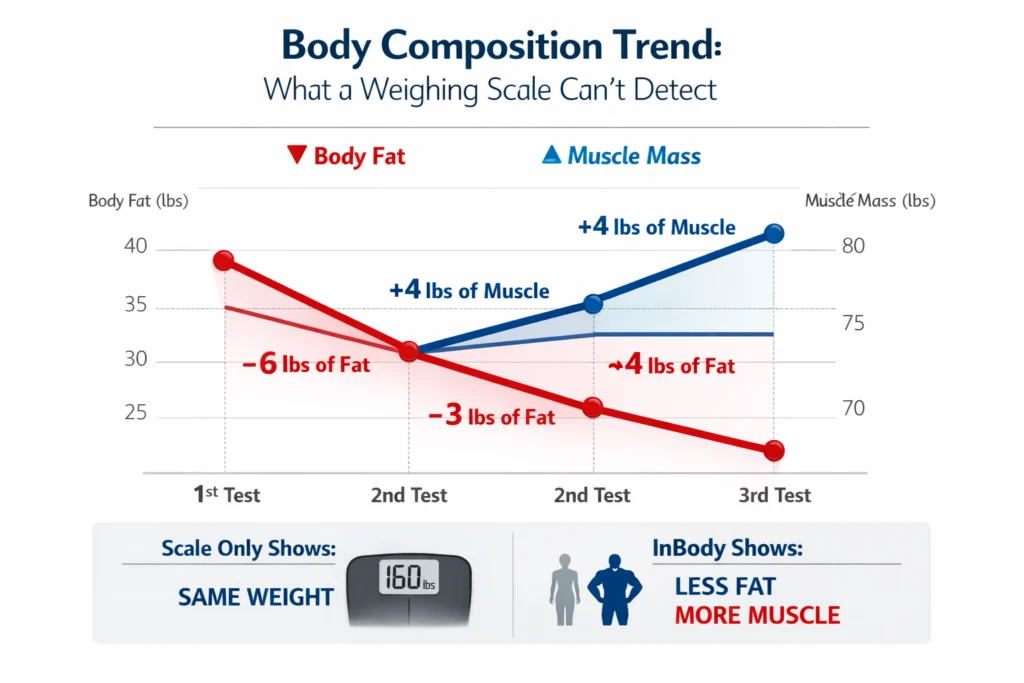
For decades, the Body Mass Index (BMI) has been the go-to metric for assessing an individual’s health based on their weight and height. However, as our understanding of health and fitness evolves, it’s becoming increasingly clear that BMI alone is not sufficient to provide a comprehensive picture of one’s overall health. Enter body composition analyzers – sophisticated tools that offer a more nuanced and accurate assessment of an individual’s physical health.
The Limitations of BMI
While BMI has been widely used due to its simplicity and ease of calculation, it has several significant drawbacks. First and foremost, BMI doesn’t distinguish between muscle mass and fat mass. This means that a muscular athlete might be classified as overweight or obese according to BMI standards despite being in excellent physical condition. Conversely, an individual with a “normal” BMI might have an unhealthy amount of body fat masked by low muscle mass.
Furthermore, BMI doesn’t account for the distribution of fat in the body. Visceral fat, which accumulates around the organs in the abdominal area, is particularly dangerous and is associated with an increased risk of various health issues, including cardiovascular disease and type 2 diabetes. BMI cannot provide information about this crucial aspect of body composition.
The Rise of Body Composition Analyzers
Body composition analyzers have emerged as a more comprehensive alternative to BMI. These devices use various technologies to measure different components of the body, including fat mass, muscle mass, bone density, and water content. By providing a detailed breakdown of these elements, body composition analyzers offer a more accurate representation of an individual’s health status.
Types of Body Composition Analyzers
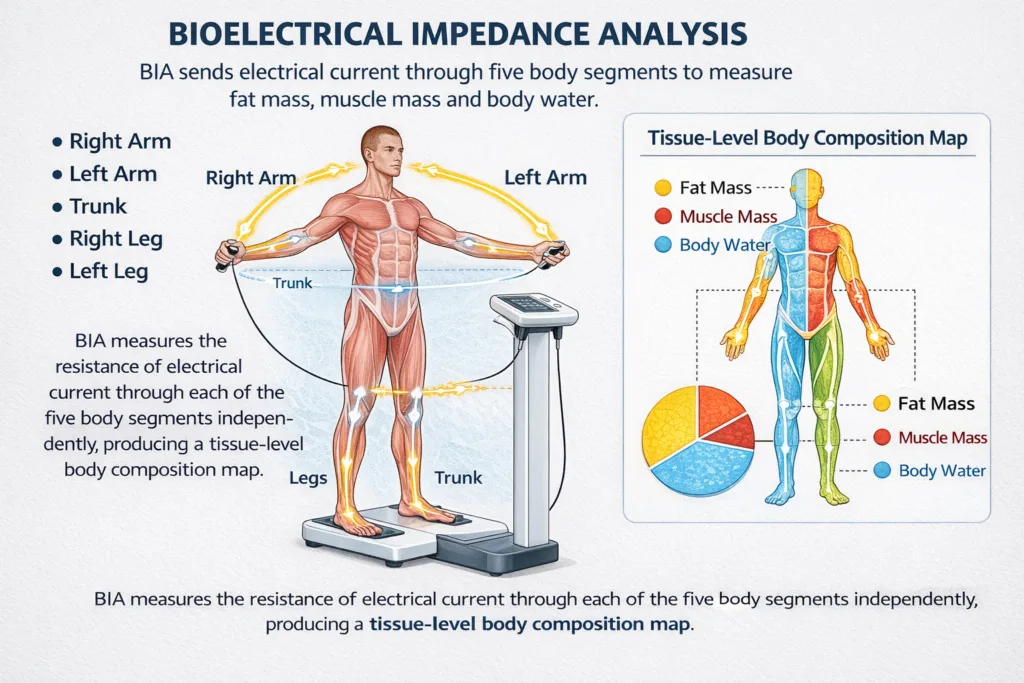
1. Bioelectrical Impedance Analysis (BIA): This method sends a low-level electrical current through the body and measures the resistance encountered. Since different tissues conduct electricity differently, BIA can estimate the proportion of fat, muscle, and water in the body.
2. Dual-Energy X-ray Absorptiometry (DEXA): Originally developed to measure bone density, DEXA scans can also assess soft tissue composition. This method uses low-dose X-rays to create detailed images of the body’s composition.
3. Air Displacement Plethysmography: This technique, often referred to as the “Bod Pod,” uses air displacement to measure body density and calculate fat and fat-free mass.
Benefits of Body Composition Analysis

1. Personalised Health Insights: By providing detailed information about an individual’s body composition, these analysers allow for more tailored health and fitness recommendations.
2. Tracking Progress: Regular body composition analysis can help individuals monitor changes in their muscle mass, fat percentage, and overall body composition over time, providing motivation and guidance for fitness goals.
3. Early Detection of Health Risks: Excessive body fat, particularly visceral fat, is associated with various health issues. Body composition analysis can identify these risks before they manifest as serious health problems.
4. Nutritional Guidance: Understanding one’s body composition can inform more effective nutritional strategies, whether the goal is weight loss, muscle gain, or overall health improvement.
5. Sports Performance Optimisation: For athletes, body composition analysis can help fine-tune training regimens and nutrition plans to optimise performance.
Interpreting Body Composition Results
While body composition analyzers provide more detailed information than BMI, interpreting the results requires some understanding of what the numbers mean. Here are some key metrics to consider:
1. Body Fat Percentage: This represents the proportion of fat mass to total body mass. Healthy ranges vary by age and gender, but generally, 10-20% for men and 18-28% for women is considered healthy.
2. Muscle Mass: Higher muscle mass is generally associated with better metabolic health and physical function. Regular strength training can help increase and maintain muscle mass.
3. Visceral Fat: This is the fat stored around the organs in the abdominal area. High levels of visceral fat are associated with increased health risks, regardless of overall body fat percentage.
4. Bone Density: This metric is particularly important for assessing the risk of osteoporosis, especially in older adults.
5. Hydration: Proper hydration is crucial for overall health and can affect the accuracy of other body composition measurements.
Limitations and Considerations
While body composition analyzers offer significant advantages over BMI, they are not without limitations. The accuracy of these devices can vary depending on factors such as hydration status, recent exercise, and even the time of day. Additionally, different types of analyzers may produce slightly different results, so it’s important to use the same method consistently when tracking changes over time.
It’s also worth noting that body composition analysis should be viewed as one part of a comprehensive health assessment.
Integrating Body Composition Analysis into Healthcare
As awareness of the limitations of BMI grows, more healthcare providers are incorporating body composition (“Body Mass Index (BMI): Learn, how it helps measure our body fat and …”) in analysis into their practice. This shift allows for more personalized health recommendations and interventions. For instance, a patient with a healthy BMI but high visceral fat might receive different advice than one with a similar BMI but with lower visceral fat and higher muscle mass.
In addition to clinical settings, body composition analyzers are becoming more accessible to the general public. Many gyms and fitness centers now offer body composition analysis services, and there are even home devices available for personal use.
Conclusion
While BMI remains a widely used tool due to its simplicity, body composition analyzers represent a significant step forward in health assessment technology. By providing a more detailed and nuanced picture of an individual’s physical makeup, these tools enable more personalized and effective approaches to health management.
As we continue to advance our understanding of health and fitness, body composition analysis will likely play an increasingly important role in both clinical practice and personal health management. By moving beyond the limitations of BMI, we can develop more accurate, personalized, and effective strategies for maintaining and improving health.
Frequently Asked Questions
Q. Why do doctors still use BMI if it is considered inaccurate?
BMI was designed in the 1830s as a tool for studying large populations, not for individual medical diagnosis. It remains popular because it is fast and requires no equipment, but it is increasingly being replaced in clinical settings by more precise technology.
Q. Can I have a “healthy” BMI and still be at risk for heart disease?
Yes. This is often called “Normal Weight Obesity.” You may have a normal weight for your height, but if your body composition shows high body fat and low muscle mass, your cardiovascular risk is similar to someone who is clinically obese.
Q. How does Body Composition Analysis actually “see” my fat and muscle?
It uses Bioelectrical Impedance Analysis (BIA), sending low-level electrical currents through the body. Because muscle contains a high percentage of water and fat does not, the device can mathematically calculate the exact volume of each tissue type.
Q. Will my body composition results change throughout the day?
Yes, results can be influenced by hydration levels, food intake, and recent exercise. For the most accurate “Beyond BMI” tracking, it is best to test in the morning, on an empty stomach, and before any strenuous physical activity.
Q. Is body composition analysis only for athletes?
Actually, it is most critical for non-athletes. While athletes use it for performance, the average person needs it to monitor “Silent Obesity,” bone mineral content, and metabolic health factors that are invisible on a standard bathroom scale.
Key Takeaways
- The BMI Blind Spot: BMI is a simple ratio of weight to height that fails to distinguish between muscle and fat. This often leads to “normal” individuals being dangerously over-fat (Skinny Fat) or athletic individuals being incorrectly labeled as overweight.
- The Visceral Fat Danger: Unlike BMI, body composition analysis measures visceral fat—the hidden fat around internal organs. This is the most accurate predictor of metabolic syndrome, heart disease, and Type 3 diabetes.
- Muscle as a Health Metric: Your health is defined more by what you have (muscle mass) than what you weigh. High muscle mass acts as a metabolic engine, whereas low muscle mass (sarcopenia) is linked to premature aging and frailty.
- Hydration and Cellular Health: Modern analysis tracks Intracellular and Extracellular water. Monitoring these levels helps identify chronic inflammation, edema, and poor nutritional status that a standard scale would never detect.
- Actionable Data Over Guesswork: Transitioning to body composition provides a “biological map.” It allows healthcare providers to create precise, data-driven interventions for nutrition and exercise rather than relying on generic weight-loss goals.

Find an InBody Scanner Near You
References & Further Reading
- PMC 2021. Association of Body Composition with T2DM: InBody 770 retrospective chart review, n=2,404. PMC8122668.
- Scientific Reports 2019. Body Composition using DEXA and T2DM: Systematic Review and Meta-Analysis — VFM odds ratios. Nature.
- Signal Transduction and Targeted Therapy 2025. Molecular signatures of skeletal muscle insulin resistance in T2DM. Nature 2025;10:320.
- World Journal of Diabetes 2024. Body composition and metabolic syndrome in T1DM — VFI, skeletal muscle mass, and insulin resistance. WJD 2024;15(1):81–91.
- PMC 2025. BMI and glycaemic control in T2DM — cross-sectional study, n=200, HbA1c correlation. PMC11853989.
- InBody BWA. Diabetes Application — clinical use of InBody for T2DM screening and management. inbodybwa.com.
- Kalra S et al. Indian Consensus on Sarcopenia including T2DM sarcopenic obesity. Int J Gen Med. 2025;18:1731–1745.
- Reviews in Endocrine and Metabolic Disorders 2025. Skeletal muscle atrophy and dysfunction in obesity and T2DM — myocellular mechanisms. Springer Nature.