Seven out of every ten Indians between 30 and 55 have poor muscle health. That is not a projection; it is the finding of the InBody-Ipsos study conducted across 1,243 adults in eight Indian cities. Yet the muscle loss driving India’s epidemics of fatigue, diabetes, and frailty continues largely unaddressed. The reason is straightforward: most people do not know which habits actually rebuild muscle, and most health assessments in India do not measure it.
This article lays out five evidence-based daily habits that measurably reverse muscle loss. Each is backed by peer-reviewed clinical data and aligned with AWGS 2019 sarcopenia guidelines. Whether you are a clinician advising patients or a patient taking charge of your own health, these habits form the most effective protocol available in preventive medicine today.
Note for Medical Practitioners
This article draws on the InBody-Ipsos 2020 study (n = 1,243 adults, 8 Indian cities, ages 30–55), published peer-reviewed sarcopenia literature, and AWGS 2019 consensus guidelines. InBody metrics referenced SMM, SMI, ECW/TBW, and PBF are produced by Direct Segmental Multi-frequency BIA at 98.4% accuracy compared to DEXA.
Why Daily Habits, Not Occasional Exercise, Determine Muscle Health
Skeletal muscle is not a static structure. It is rebuilt and broken down continuously, a process called muscle protein turnover, and it responds directly to daily inputs: the protein you consume, the mechanical load you place on it, and the hormonal and inflammatory environment you maintain. This means that single interventions or occasional efforts produce minimal long-term results. What matters is consistency over weeks and months.
The clinical significance of this is substantial. Skeletal muscle accounts for approximately 80% of insulin-stimulated glucose uptake. When muscle mass falls, the body’s primary glucose disposal mechanism is compromised independently of body weight or BMI. Additionally, muscle acts as the body’s primary reservoir of glutamine, which fuels the immune system’s lymphocytes and macrophages. Low muscle mass is therefore not simply a fitness deficit. It is a systemic metabolic liability with measurable consequences for diabetes risk, immune function, cardiovascular health, and functional independence.
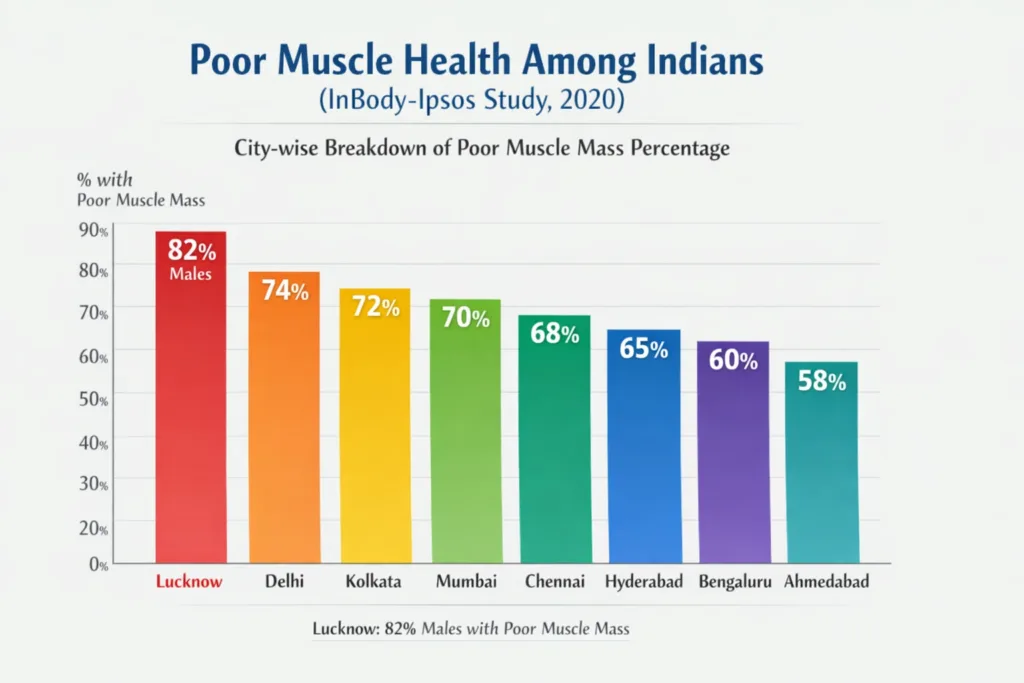
The Indian Phenotype Makes Muscle Loss Invisible
Research by Professor C.S. Yajnik at KEM Hospital, Pune, established that South Asians, including Indians, carry significantly less muscle and more visceral fat at the same body weight compared to Western populations. This “thin-fat” phenotype means that an Indian adult with a BMI of 23 may be clinically low in skeletal muscle while appearing entirely healthy on standard assessments.
Standard weighing scales and BMI cannot detect this. InBody’s Direct Segmental Multi-frequency BIA, however, measures skeletal muscle mass in kilograms directly within 60 seconds. It is the only practical clinical tool that makes the invisible visible.
The 5 Daily Habits That Clinically Reverse Muscle Loss
1. Hit Your Protein Target at Every Meal, Not Just Once a Day
No other single habit has a greater impact on muscle health than consistent, adequate protein intake. The minimum clinical target for a healthy Indian adult is 1.0 g of protein per kilogram of body weight per day. For adults over 40, or anyone actively rebuilding muscle, the target rises to 1.2–1.6 g/kg/day. For a 70 kg Indian adult, this means 70–112 g of protein daily — roughly double what most Indians currently consume.
Critically, protein must be distributed across all three meals, not concentrated in a single sitting. Muscle protein synthesis (MPS) responds to per-meal amino acid exposure. A single 80 g protein meal does not produce the same anabolic effect as three meals providing 25–30 g each. This single habit change, distributing protein across meals, produces measurable differences in InBody skeletal muscle mass readings within 8–12 weeks.
Best protein sources for Indian diets
Complete proteins containing all nine essential amino acids are most effective at stimulating MPS. For Indian adults, the most practical high-quality options are: eggs (the nutritional benchmark for complete protein), paneer, curd, chicken, fish, soya chunks, and dal combined with rice or roti. Whey protein supplementation is a clinically valid and cost-effective option for individuals who cannot consistently hit targets through food alone.
1.0–1.6 g / kg/day distributed across 3 meals, 25–30 g per meal minimum, Complete proteins preferred
2. Commit to Progressive Resistance Training Three Times Per Week
Resistance training is the most powerful stimulus for skeletal muscle protein synthesis, available, more effective than any supplement, medication, or dietary change alone. The minimum effective dose for measurable muscle gain in previously sedentary Indian adults is three sessions per week of 30–40 minutes each, incorporating compound movements that load large muscle groups simultaneously.
You do not need a gym. Bodyweight exercises, such as squats, lunges, push-ups, hip hinges, step-ups, and planks, provide sufficient mechanical load to drive meaningful muscle protein synthesis in deconditioned individuals. The critical principle is progressive overload: systematically increasing the challenge by adding repetitions, sets, or resistance over time. Without progression, adaptation plateaus within 6–8 weeks and muscle gains stall.
Resistance training also produces benefits that extend well beyond muscle mass. It reduces visceral fat, improves insulin sensitivity, strengthens bone mineral density, lowers resting blood pressure, and significantly reduces cardiovascular risk, all of which are particularly relevant to the Indian metabolic profile. In patients with borderline fasting glucose or prediabetes, it is now recognised as a first-line clinical intervention, not an optional lifestyle choice.
3 sessions/week, 30–40 min per session, Compound movements, Progressive overload essential. Bodyweight is sufficient to start.
3. Measure Muscle Mass: Directly Replace Your Weighing Scale With an InBody Scan
Why Measuring Muscle Matters
You cannot improve what you do not measure. This is especially true for muscle mass. Most Indians rely on weighing scales and BMI to track their health. However, these tools cannot detect muscle properly.
In fact, BMI can be misleading. It increases when you gain muscle and decreases when you lose it. As a result, it may show negative progress even when your body composition is improving.
Why InBody Analysis Is More Accurate
InBody body composition analysis provides a clearer picture. It measures skeletal muscle mass directly in kilograms. It also compares your results with age- and sex-adjusted Indian population norms.
A single scan takes less than 60 seconds. Moreover, it requires no radiation, no blood tests, and no specialist interpretation.
The report includes:
- Skeletal Muscle Mass (SMM)
- Skeletal Muscle Index (SMI) for AWGS sarcopenia screening
- Segmental Lean Analysis (for each limb)
- Visceral Fat Level (VFL)
- ECW/TBW ratio (for inflammation)
- InBody Score
Why Regular Tracking Is Important
Tracking once is not enough. Instead, regular monitoring gives meaningful insights.
Serial scanning every 8–12 weeks helps track progress objectively. It also improves motivation and consistency. In addition, it allows early detection of plateaus or muscle loss.
In Indian clinical and corporate wellness settings, patients who understand their InBody Score show better compliance. They follow nutrition and exercise plans more consistently than those tracking only weight.
Simple Tracking Guidelines
- Scan every 8–12 weeks
- Track SMM against age norms
- Monitor SMI against AWGS threshold
- Focus on leg segment muscle specifically
Clinical Protocol: Recommended InBody Monitoring Schedule
For Indian adults aged 30 and above, the following schedule supports proactive muscle health:
- Baseline scan: At first consultation or annual health check
- 3-month scan: Evaluate response to diet and exercise
- 6-month scan: Confirm sustained muscle gain and fat loss
- Annual scan: Monitor long-term metabolic health
Key Markers to Track at Every Visit
- InBody Score trend
- SMM vs age norm
- SMI vs AWGS threshold
- Segmental Lean Analysis (especially legs)
- ECW/TBW ratio
4. Address Vitamin D, Magnesium, Zinc, and B12 Deficiencies
Resistance training and protein are the primary drivers of muscle gain, but micronutrient deficiencies act as a significant brake on that process. Vitamin D, magnesium, zinc, and vitamin B12 are all directly involved in muscle protein synthesis and neuromuscular function. In India, all four are highly prevalent as deficiencies, and correcting them measurably accelerates the rate of muscle recovery when combined with the first two habits.
Vitamin D is particularly consequential. Vitamin D receptors are present in muscle cells, and deficiency leads to reduced Type II muscle fibre size, the fast-twitch fibres responsible for strength and power output. Despite India’s abundant sunlight, an estimated 50–90% of Indian adults are Vitamin D deficient, due to indoor lifestyles, dark skin pigmentation reducing cutaneous synthesis, and very low dietary Vitamin D sources in typical Indian food.
Magnesium is required for ATP synthesis, the biochemical process that powers all muscular contraction. Deficiency reduces the capacity for both muscle contraction and recovery. Zinc is directly involved in muscle protein synthesis and IGF-1 signalling. Vitamin B12 deficiency is extremely common in vegetarian and semi-vegetarian Indian diets, causing neuromuscular dysfunction that directly limits resistance training capacity and therefore muscle adaptation.
Clinical recommendation
A basic micronutrient panel, including Vitamin D (25-OH), serum magnesium, serum zinc, and serum B12, should accompany any body composition assessment in Indian adults presenting with low muscle mass or fatigue. Correcting identified deficiencies before or alongside a resistance training programme substantially accelerates measurable results.
Check Vitamin D (25-OH), Serum B12, Magnesium, Zinc.
5. Track Your InBody Score and Make It Your Primary Health Benchmark
Long-term habit change requires a feedback loop. The InBody Score, a composite 0–100 index of overall muscle-fat balance, provides exactly that. A score above 80 indicates healthy body composition. Scores below 70 indicate a clinically relevant imbalance: typically too much fat, too little muscle, or both simultaneously.
What makes the InBody Score particularly valuable as a behavioural tool is that it responds to both dimensions of intervention simultaneously. If you gain muscle but also gain fat, the score reflects that nuance. If you lose fat but also lose muscle, a common and counterproductive outcome of calorie restriction without resistance training, the score catches that too. It therefore aligns patient behaviour precisely with what matters clinically: improving muscle-fat balance, not just reducing the number on a weighing scale.
In Indian clinical practice, where patient compliance and follow-up are among the most significant barriers to achieving lasting health outcomes, the InBody Score functions as a powerful motivational tool. Patients who can see a single number improving over serial scans show measurably better adherence to both nutrition and exercise programmes than those tracking weight or BMI alone.
Target: Score above 80
Below 70 = clinical concern
Tracks both muscle AND fat
Use as a primary health KPI
Real Clinical Case: 16 Weeks, Five Habits, Measurable Reversal
A 44-year-old male IT professional in Bengaluru presented to a corporate wellness clinic with persistent fatigue, mild lower back pain, and borderline fasting glucose of 101 mg/dL. His BMI was 24.2, entirely normal by standard criteria. He had never been flagged for metabolic risk in any previous health assessment.
An InBody 770 scan produced a different clinical picture. His Skeletal Muscle Mass was 4.1 kg below the population norm for his age and height. Skeletal Muscle Index of 6.8 kg/m² fell below the AWGS sarcopenia threshold of 7.0 kg/m². His Visceral Fat Level was 11 (high-risk range), and his ECW/TBW ratio of 0.391 indicated subclinical inflammation. In other words, he met clinical criteria for sarcopenia at 44, with a normal BMI and no prior detection.
A 16-week programme was initiated based on all five habits described above: resistance training three times per week, dietary protein increased to 1.4 g/kg/day using eggs, paneer, and whey protein, Vitamin D supplementation following a confirmed deficiency, and InBody scans at 8 and 16 weeks to track progress. The 16-week results were clinically significant across every tracked marker.
- 16-Week Outcomes Body Composition Analysis
- +3.2 kg Skeletal Muscle Mass gained
- 7.4 SMI kg/m² is now above the AWGS sarcopenia threshold
- ↓ 3 Visceral Fat Level (11 → 8)
- 94 mg/dL Fasting glucose returned to the normal range
His fatigue resolved completely. His lower back pain improved as a direct consequence of restored core and lower limb muscle mass. This case reflects a pattern seen consistently across Indian clinical and corporate wellness settings: muscle loss is widespread, largely undetected, and highly reversible when identified early and addressed with the right combination of five consistent habits.
What InBody Measures and Why Blood Tests Cannot Replace It
Standard health check-ups in India, even at premium corporate wellness programmes, measure weight, BMI, and blood markers. None of these detects skeletal muscle mass directly. The table below maps each consequence of low muscle mass to the InBody marker that identifies it and the blood test that cannot.
| Clinical Consequence | Mechanism | InBody Marker | Detectable by Blood Test? |
|---|---|---|---|
| Type 2 Diabetes Risk | 80% of glucose uptake is muscle-dependent low SMM = insulin resistance | Skeletal Muscle Mass (SMM) | ❌ Not directly |
| Sarcopenia and Frailty | SMI below AWGS threshold → loss of strength and functional independence | Skeletal Muscle Index (SMI) | ❌ No blood test measures SMI |
| Visceral Fat Accumulation | Lower BMR from muscle loss → fat replaces muscle compartment | Visceral Fat Level (VFL) | ❌ Triglycerides are an indirect proxy only |
| Chronic Fatigue | Insufficient myokine output and reduced cellular energy capacity | ECW/TBW Ratio | ❌ CBC misses sub-clinical inflammation |
| Falls and Fractures | Reduced leg muscle mass → impaired balance and load-bearing capacity | Segmental Lean Analysis: Legs | ❌ DEXA measures bone, not segmental muscle |
| Immune Dysfunction | Muscle is the primary glutamine reservoir for lymphocytes and macrophages | SMM + ECW/TBW Ratio | ❌ Lymphocyte count does not identify the cause |
Who Should Be Screened Immediately
Given that 71% of Indians already have poor muscle health, a baseline InBody body composition scan is advisable for almost all adults over 30. The following groups have the highest clinical priority for immediate screening and intervention.
- Adults over 30 with sedentary occupations
IT professionals, office workers, and others with minimal daily physical activity are at the highest risk of progressive disuse atrophy. Muscle loss in this group often remains asymptomatic until the loss is clinically significant. - Patients with prediabetes or Type 2 diabetes
Low muscle mass both causes and accelerates insulin resistance. Body composition monitoring should be standard in every diabetic patient’s care plan, not an optional add-on. - Patients with unexplained fatigue, weakness, or reduced exercise tolerance
These are frequently the first symptoms of muscle loss in the 40–60 age group, and are routinely missed by standard blood panels, including CBC and thyroid function. - All adults over 50
The rate of muscle loss accelerates sharply after 50. Sarcopenia screening using InBody SMI data should be integrated into all preventive health assessments in this age group as a standard of care. - Post-surgical and post-illness patients
Hospitalisation, bed rest, and reduced oral intake drive rapid muscle loss. Serial InBody monitoring during rehabilitation tracks recovery and guides nutritional support precisely. - Women post-menopause
Oestrogen plays a protective role in muscle mass maintenance. Its withdrawal at menopause accelerates muscle loss significantly, making this group a high-priority target for proactive body composition monitoring.

Key Takeaways for Clinicians and Patients
- 71% of Indians aged 30–55 have clinically poor muscle health — confirmed by the InBody-Ipsos study of 1,243 adults across 8 Indian cities in 2020.
- Low skeletal muscle mass is an independent risk factor for Type 2 diabetes, sarcopenia, immune dysfunction, and cardiovascular disease, not merely a fitness concern.
- BMI and weighing scales cannot detect muscle loss. InBody body composition analysis measures skeletal muscle mass directly, in kilograms, against age- and sex-adjusted Indian population norms.
- The five habits that reverse muscle loss are: hit your daily protein target · do resistance training three times per week · measure with InBody every 8–12 weeks · correct micronutrient deficiencies · track your InBody Score as your primary health benchmark.
- Muscle loss is highly reversible with consistent habits producing measurable InBody gains of 1.5–3.5 kg of skeletal muscle mass within 12–24 weeks.
- The results extend far beyond muscle: fasting glucose, visceral fat, fatigue, and physical function all improve measurably as skeletal muscle mass is restored.
Frequently Asked Questions
Q. Which of the five habits has the greatest single impact on muscle health?
Consistent protein intake and resistance training are equally essential; neither works well without the other. However, if patients can implement only one habit immediately, protein distribution across three daily meals tends to produce the fastest early measurable improvement in skeletal muscle mass on InBody scans, particularly in individuals who are severely protein-deficient, which describes the majority of the 71% identified in the InBody-Ipsos study.
Q. Can muscle loss be reversed after 50 or 60?
Yes. Skeletal muscle responds to resistance training and adequate protein at any age. Adults over 50 show slower adaptation than younger individuals, but measurable InBody gains are consistently observed within 12–16 weeks of consistent effort. The AWGS 2019 guidelines explicitly endorse resistance training as the primary intervention for sarcopenia across all age groups, including those over 70.
Q. Is it possible to have low muscle mass at a normal body weight?
Yes, and this is exactly the clinical challenge the InBody-Ipsos study highlighted. The “thin-fat” Indian phenotype, documented by Professor C.S. Yajnik, means that many Indian adults have clinically low skeletal muscle mass alongside elevated visceral fat while maintaining a completely normal BMI. Standard health assessments miss this entirely. The InBody scan is currently the only practical clinical tool that detects it directly.
Q. How quickly will I see results on an InBody scan?
Measurable increases in skeletal muscle mass typically appear within 8–12 weeks of consistent resistance training combined with adequate protein intake (1.2–1.6 g/kg/day). Most individuals below the population norm gain approximately 1.5–3.5 kg of skeletal muscle mass over 12–24 weeks. The InBody scan at 8 weeks is an important motivational checkpoint, as measurable changes at this stage strongly predict continued adherence.


