Fitness 8 min read
Obesity vs Overweight: What’s the Difference & Why It Matters
Obesity and overweight occur when the number of fat cells in the body increases. Several factors cause this condition, including unhealthy eating habits, lack of sleep, and certain…
Reading about body composition? Find an InBody test centre near you →
Obesity and overweight occur when the number of fat cells in the body increases. Several factors cause this condition, including unhealthy eating habits, lack of sleep, and certain medications. A high level of body fat is common worldwide and leads to many health problems. Genetics also plays a role in increasing body fat levels.
While overweight refers to excess fat accumulation, obesity is a chronic disease with serious health risks. These risks include type 2 diabetes, osteoarthritis, cancer, and cardiovascular diseases. In addition, many people experience mental stress.
Doctors calculate obesity and overweight using the Body Mass Index (BMI). They use the formula:
BMI = weight (kg) / [height (m)]²
Based on BMI, they classify individuals into four categories: underweight, normal weight, overweight, and obese.
- Underweight: BMI<18.5
- Normal weight: BMI 18.5 – 24.9
- Overweight: BMI 25 – 29.9
- Obese: BMI>=30

Health implications and health risks
Obesity and overweight have numerous health implications and risks. Some of them are listed below:
- Cardiovascular Diseases: Diseases such as heart stroke, attack, high blood pressure, and coronary artery disease. These health hazards are directly linked to excessive fat content in a person’s body. Health implications such as high cholesterol, inflammation, triglycerides, and insulin resistance are contributors to cardiovascular complications.
- Type 2 Diabetes Mellitus: Type 2 diabetes mellitus is a condition in which your body muscles and tissues tend to get resistant toward your insulin hormone. This is caused by the high amount of fat deposited in your body and because of this patients with high blood sugar need to be injected with external insulin.
- Cancer: Cancer is another health risk that is caused due to excessive fat deposits in the human body. Due to these excessive fats, your body produces a high level of growth hormones. Growth hormones are responsible for cell division and mutation, and this causes rapid division of cells. Cancers such as breast cancer, colon cancer, prostate cancer, endometrial cancer, pancreatic cancer, and ovarian cancer are some of the cancers that are caused by obesity and overweight.
- Respiratory Diseases: Excessive fat is responsible for the decrease in lung capacity to store oxygen, and resistance in air passage. Various respiratory diseases such as sleep apnea, asthma, and hypoventilation syndrome.

Common causes of obesity and overweight
Both obesity and overweight are a state of excessive fat. This is due to various causes such as diet, physical activity, genetics, environment, and psychological & behavioral factors. Let’s discuss them in brief.
- Diet: A diet with a high-calorie intake is not good for health and seriously affects overall health.
- High-Calorie Intake: Foods like fast food, deep-fried snacks, excessive sugar, and processed or canned foods contain high calories. These are high-energy foods. Consuming more fat than what is burnt will leave fat in your body.
- Low-quality diet: Promotors of fat are carbohydrates, sugar, and fats such as trans-fat and saturated. A low-quality diet can also be a diet that has no fruits, vegetables, proteins, etc.
- Irregular eating habits: Irregular eating habits have consequences like overweight and obesity. Due to irregular eating habits, overall calorie intake increases. Skipping a meal results in immense hunger, resulting in overeating at the time of the next meal.
- Lack of Physical Activities: Physical exercise helps your body to convert calories into energy. It also helps increase metabolism.
- Sedentary Lifestyle: Modern lifestyle has become busy. Long working hours and sitting throughout the day are a trend. People have insufficient physical activity, which reduces calorie burn and results in excessive fat deposits in the body.
- Lack of Exercise: Due to a tight schedule, individuals are not able to get time for gym, physical activities, walking/jogging, or any recreational activities. This schedule has affected the metabolism of human beings and due to this fat burn has taken a step back.
- Genetics, and Family: Although genetics does not play a vital role in obesity and overweight, there is a slight chance of it happening.
- Genetics: Genetics can be ignored while checking for causes of obesity or overweight conditions as genes can never show the full story. It all depends on the activities and food habits of an individual. People might think a person might get overweight or obese by looking at family history and vice versa but this is not always true. Although children adapt to what they are taught or observe, yet still cannot define their body structure.
- Family Dynamics: Eating habits, patterns, and attitudes of the family towards what they eat and what they do not are driving factors towards calorie intake. Whether they do physical activities such as gym, walking, or jogging is also considered.
- Sleep: Sleep is a contributing factor in calorie burn. Poor quality of sleep messes up hormones that are responsible for the regulation of appetite.
- Hormonal Imbalance: Due to lack of sleep or poor quality of sleep, individuals might face hormonal imbalances that help in appetite regulation. Lack of sleep or sleep deprivation can increase hunger resulting in more consumption of food with high-calorie or overeating.
- Alerted Metabolic Function: Less sleep or poor quality of sleep can affect metabolism negatively, including insulin sensitivity, insulin resistance, and glucose metabolism. This might increase the risk of weight gain around your abdominal area.

Although both overweight and obesity are different, they come with numerous health implications out of which some are severe, and some are chronic. Obesity and overweight are caused by habits such as the consumption of high-calorie diets, low-quality diets, irregular eating patterns, genetics, and lack of physical activities. To maintain a healthy lifestyle, an individual should include best practices such as healthy & timely eating, getting adequate sleep, and physical activities in their daily routine to stay fit and not gain fat. By these practices, a person can mitigate the risk of health problems that come with excess weight and improve overall health.
Frequently Asked Questions
Q. What is the actual difference between being “overweight” and being “obese”?
While both terms refer to carrying excess body fat, “overweight” is generally defined as having an excess deposit of fat, whereas “obesity” is classified as a chronic disease. Obesity typically involves a higher volume of fat cells and carries a much higher risk of severe, long-term health complications.
Q. How do I know which category I fall into?
The blog explains that the Body Mass Index (BMI) is the standard tool used for categorization. You can calculate it by dividing your weight (kg) by your height in meters squared ($BMI = kg/m^2$):
Obese: 30 or higher
Normal weight: 18.5 – 24.9
Overweight: 25 – 29.9
Q. Can lack of sleep really make me gain weight?
Yes. Poor sleep quality or sleep deprivation messes with the hormones responsible for regulating your appetite. This hormonal imbalance often increases hunger and cravings, leading to higher calorie consumption. Additionally, lack of sleep can negatively affect your metabolism and insulin sensitivity.
Q. Why does obesity increase the risk of cancer?
Excessive fat deposits cause the body to produce higher levels of growth hormones. These hormones are responsible for cell division; when they are overproduced, it can lead to rapid cell division and mutations, increasing the risk of cancers such as breast, colon, pancreatic, and ovarian cancer.
Q. Is obesity purely a matter of genetics?
Not necessarily. While genetics can play a slight role, the blog emphasizes that genes do not tell the full story. Body structure and weight are primarily driven by an individual’s daily activities, eating habits, and family dynamics (such as the types of food served at home and the family’s attitude toward exercise).
Key Takeaways
- 1 in 4 Indians has obesity (NFHS-5), and BMI misses nearly half of them. Normal weight obesity is present in 48.7% of normal-BMI Indian adults in recent studies. Body composition technology detects what BMI cannot.
- The 7 proven ways body composition technology transforms obesity treatment all require InBody data. BMI and scale weight cannot provide visceral fat level, body fat percentage, muscle mass, ECW/TBW ratio, or phase angle, the metrics that actually define and track obesity.
- The Endocrine Society of India defines obesity as body fat above 25% in men, above 30% in women. Using these thresholds transforms how many Indian patients are correctly identified and treated.
- GLP-1 agonists and SGLT-2 inhibitors can cause significant lean mass loss alongside fat loss. Only InBody confirms whether treatment is producing beneficial fat reduction enabling immediate dietary and exercise adjustment if needed.
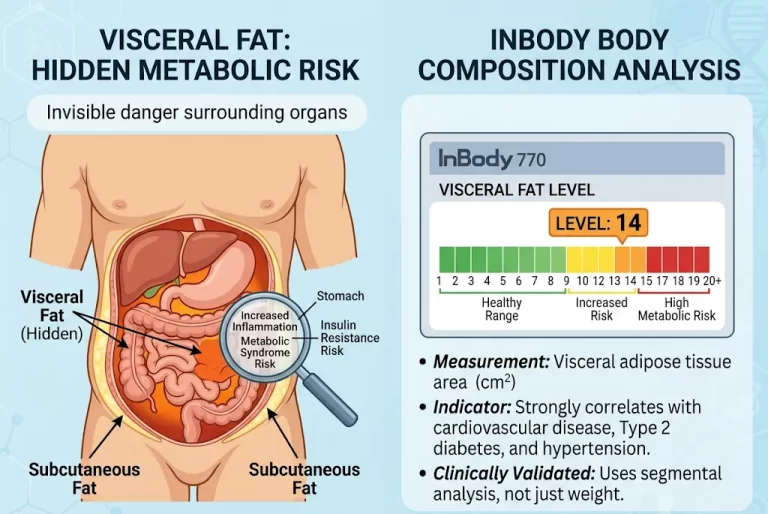
- Visceral fat reduction, not total weight loss, is the primary goal for improving metabolic health. InBody’s direct VFL measurement tracks the fat driving T2DM, MASLD, CVD, and hypertension and confirms that it is declining.
- InBody delivers all 7 obesity-relevant metrics: body fat %, VFL, VFA, SMM, ECW/TBW ratio, phase angle, and InBody Score in under 60 seconds, at every clinic visit, without radiation, blood draws, or specialist equipment.
Detect the Obesity That BMI Cannot See
An InBody scan takes under 60 seconds. It measures body fat percentage, visceral fat level, muscle mass, and cellular health, and identifies normal-weight obesity. It tracks treatment progress. And it confirms your obesity programme is producing the right metabolic changes, not just scale weight loss.
Find an InBody Scanner Near You
References & Further Reading
- PMC 2021. Association of Body Composition with T2DM: InBody 770 retrospective chart review, n=2,404. PMC8122668.
- Scientific Reports 2019. Body Composition using DEXA and T2DM: Systematic Review and Meta-Analysis — VFM odds ratios. Nature.
- Signal Transduction and Targeted Therapy 2025. Molecular signatures of skeletal muscle insulin resistance in T2DM. Nature 2025;10:320.
- World Journal of Diabetes 2024. Body composition and metabolic syndrome in T1DM — VFI, skeletal muscle mass, and insulin resistance. WJD 2024;15(1):81
- InBody BWA. Diabetes Application — clinical use of InBody for T2DM screening and management. inbodybwa.com.
- Kalra S et al. Indian Consensus on Sarcopenia including T2DM sarcopenic obesity. Int J Gen Med. 2025;18:1731–1745.