
The COVID-19 pandemic changed how we think about immunity in young people. For the first time, clinicians, parents, and educators faced an uncomfortable truth. Being young does not always mean being protected.
In fact, recent evidence shows that body composition plays a key role in health. This includes fat mass, muscle mass, and body water. These factors directly affect immune response. They also influence the risk of severe illness and long-term chronic disease.
As a result, the question is no longer just, “Is my child at a healthy weight?” Instead, a more important question is: “What is my child’s body made of?” And more importantly, is that composition supporting or weakening their immunity?
In this article, we explain the science behind body composition and youth immunity. We also show why common tools like BMI miss critical insights. Finally, we explore how the InBody H30 provides precise results in under 60 seconds for clinicians, schools, and families.
| 80% of insulin-stimulated glucose uptake occurs in skeletal muscle making muscle mass a direct immunity factor | 60 sec Time for a complete InBody H30 body composition scan for children and adolescents | 20+ Parameters measured by the InBody H30 including growth charts, fat mass, and muscle mass | 101M Indians living with Type 2 diabetes a comorbidity that severely worsens COVID-19 outcomes |
Why COVID-19 Made Youth Body Composition a Medical Priority
When COVID-19 emerged, the early data appeared reassuring for younger populations. Children and adolescents, the evidence suggested, were less likely to develop severe disease than older adults. However, as the pandemic progressed, a more nuanced picture emerged. Specifically, researchers found that youth with poor body composition, characterised by excess body fat, low muscle mass, or elevated visceral fat, faced significantly worse outcomes than their lean, well-nourished peers.
Furthermore, the indirect effects of the pandemic on youth health proved just as damaging as the virus itself. School closures, reduced physical activity, disrupted meal patterns, and increased screen time all contributed to measurable deterioration in the body composition of children and adolescents across India. As a result, a generation of young people entered the post-pandemic period with higher fat mass, lower muscle mass, and weaker metabolic foundations than before.
Comorbidities Are No Longer Just an Adult Problem
Traditionally, conditions like obesity, insulin resistance, and metabolic syndrome were considered adult diseases. Nevertheless, that assumption no longer holds. Evidence from multiple Indian and global studies shows that adolescents with high body fat percentages and low skeletal muscle mass are already developing the metabolic precursors of Type 2 diabetes and cardiovascular disease, the very comorbidities that made COVID-19 so dangerous in adults.
Moreover, the inflammatory state associated with excess body fat, particularly visceral fat, directly suppresses immune function. In other words, a child with poor body composition does not just face a higher risk of metabolic disease in adulthood. They also face a compromised immune response right now, when it matters most.
CLINICAL INSIGHT FOR MEDICAL PROFESSIONALS
Body composition assessment in adolescents serves a dual clinical purpose. First, it identifies those at immediate immunological risk, high fat mass and low muscle correlate directly with reduced T-cell activity and elevated pro-inflammatory cytokine levels. Second, it provides an early-warning system for chronic disease onset. Body composition changes during puberty are among the strongest predictors of adult metabolic health. Therefore, integrating routine body composition screening into school and clinic-based health programmes is now a clinical imperative, not an optional enhancement.
Why BMI Fails Children and Adolescents Especially in India
BMI remains the most commonly used metric for assessing weight status in children and adolescents in India. However, its limitations are especially pronounced in young, growing populations and particularly in South Asian children, whose body composition differs significantly from that of Western populations on which BMI reference ranges were originally calibrated.
The Thin-Fat Indian Child
Research by Professor C.S. Yajnik and colleagues at KEM Hospital Pune has demonstrated that Indian children and adolescents characteristically exhibit high body fat and low muscle mass relative to their body weight a pattern that persists into adulthood and is directly associated with early-onset insulin resistance and metabolic disease. Consequently, an Indian adolescent with a BMI in the “healthy” range may simultaneously carry a body fat percentage that would be classified as obese by composition standards.
Furthermore, BMI cannot distinguish the rapid, normal fluctuations in muscle mass, bone mass, and fat mass that occur during puberty. As a result, it is a particularly unreliable tool during precisely the developmental window when accurate body composition data matters most adolescence.
| What Clinicians Need to Know | BMI Tells You | InBody H30 Tells You |
|---|---|---|
| Is fat mass within healthy range? | No, weight only, no fat detail | Yes, precise fat mass in kg and % with age/gender norms |
| Is muscle mass adequate for age? | No, cannot measure muscle | Yes, skeletal muscle mass vs growth chart norms |
| Is growth trajectory healthy? | Partial weight for age only | Yes, growth graphs for all key composition parameters |
| Is the child at metabolic risk? | No, misses thin-fat phenotype | Yes, visceral fat, ECW/TBW ratio, obesity analysis |
| Is immunity likely compromised? | No | Indicative high fat + low muscle flags immune risk |
| Are results India-specific? | No, Western reference ranges | Yes, Asian-calibrated reference values applied |

The Science: How Body Composition Directly Affects Immune Function
The relationship between body composition and immune function is well-established in the clinical literature. Specifically, three body composition components fat mass, skeletal muscle mass, and body water distribution each play distinct roles in determining how effectively the immune system responds to pathogens like SARS-CoV-2.
Fat Mass: How Excess Body Fat Suppresses Immunity
Adipose tissue, particularly visceral fat surrounding the abdominal organs, is metabolically active. It secretes a range of pro-inflammatory cytokines, including IL-6, TNF-α, and leptin, which chronically activate the immune system. As a result, children and adolescents with high fat mass exist in a state of persistent, low-grade inflammation. Consequently, when a genuine immune challenge like COVID-19 arrives, the immune system’s capacity for a targeted, proportionate response is already compromised.
Moreover, excess fat mass in adolescents is associated with reduced vaccine efficacy. Research has demonstrated that obese individuals show lower antibody titres following vaccination compared to lean individuals a finding directly relevant to COVID-19 vaccination programmes in young people. In other words, addressing body composition in youth is not just a long-term health goal. It is an immediate immunological priority.
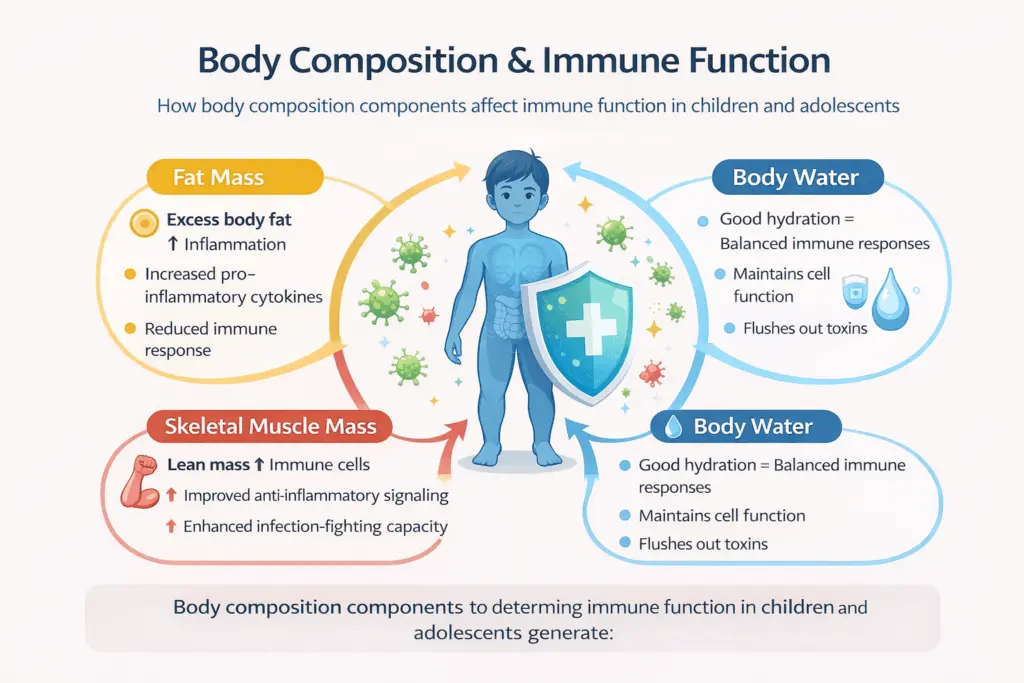
Skeletal Muscle Mass: The Immune System’s Fuel Reserve
Skeletal muscle plays a role in immunity that goes far beyond physical strength. During infection, the immune system requires large quantities of amino acids, specifically glutamine, to fuel the proliferation of immune cells. The primary source of these amino acids is skeletal muscle. Therefore, a child or adolescent with low skeletal muscle mass has a fundamentally reduced capacity to sustain an immune response over the course of an illness.
In addition, skeletal muscle is responsible for approximately 80% of insulin-stimulated glucose uptake. This means that low muscle mass is a direct risk factor for insulin resistance which itself impairs immune function by disrupting the signalling pathways that regulate T-cell and B-cell activity. As a result, the muscle-immunity connection operates on multiple levels simultaneously.
CLINICAL ALERT: LOW MUSCLE MASS IN INDIAN ADOLESCENTS
India faces a dual crisis in youth body composition: excess fat and insufficient muscle, occurring simultaneously a condition known as sarcopenic obesity. Driven by protein-deficient diets, sedentary lifestyles, and reduced outdoor activity (accelerated by pandemic lockdowns), sarcopenic obesity in Indian adolescents is a direct risk factor for both impaired immune response and early-onset metabolic disease. Standard BMI screening misses this entirely. Only direct body composition measurement can identify it.
Body Water Distribution: The ECW/TBW Ratio as an Inflammation Marker
The ECW/TBW ratio, the ratio of extracellular water to total body water, serves as a sensitive marker of systemic inflammation and cellular health. A healthy ratio in children and adolescents is below 0.380. However, ratios at or above 0.390 indicate an inflammatory or nutritionally compromised state. Notably, this ratio is elevated in children with malnutrition, chronic illness, and post-viral recovery states, all of which are clinically relevant in the post-COVID landscape.
Furthermore, the ECW/TBW ratio responds to nutritional interventions faster than other biomarkers making it a uniquely valuable tool for monitoring whether dietary changes are having a genuine physiological effect in young patients. Consequently, clinicians using the InBody H30 can track not just whether a child is getting better, but whether the cellular environment is shifting toward health.
Body Composition During Puberty: Why This Window Is Critical
Puberty represents the most significant period of body composition change in human development and the window during which adult metabolic health is most decisively shaped. During puberty, fat mass, lean body mass, and bone mineral content all undergo rapid, age-correlated transformations. As a result, the body composition trajectory established during adolescence is one of the strongest predictors of adult health outcomes.
Specifically, research demonstrates that adolescents who exit puberty with high fat mass and low muscle mass carry those patterns into adulthood with a high degree of tracking, meaning the fat-to-muscle ratio established during these years tends to persist and worsen over time. Moreover, the metabolic changes of puberty, including the temporary insulin resistance that naturally occurs during mid-puberty, make this period a window of heightened vulnerability to the compounding effects of poor diet, inactivity, and excess fat accumulation.
Gender Differences in Pubertal Body Composition
Body composition trajectories during puberty differ significantly between boys and girls, a distinction that standard BMI-for-age charts handle poorly. In boys, puberty is characterised by a pronounced increase in skeletal muscle mass driven by testosterone. In girls, by contrast, puberty typically increases fat mass, particularly subcutaneous fat. Consequently, a single BMI reference range cannot meaningfully assess both sexes during this developmental period.
The InBody H30 applies gender-specific reference values and generates separate growth charts for boys and girls, ensuring that assessments are clinically meaningful for each patient, not just statistically average across both groups. Furthermore, these reference charts allow clinicians and parents to track composition changes longitudinally across multiple scans, providing a genuine developmental picture rather than a single snapshot.

The InBody H30: Clinical-Grade Body Composition for Children and Adolescents
The InBody H30 is specifically designed for use with children and adolescents. Unlike standard adult body composition devices, it applies paediatric-specific algorithms and reference ranges, ensuring that results are clinically meaningful for growing bodies at every stage of development. Furthermore, the scan is completely non-invasive and takes under 60 seconds, making it practical for use in schools, clinics, and community health programmes.
How the InBody H30 Works
The InBody H30 uses Direct Segmental Multi-frequency Bioelectrical Impedance Analysis (DSM-BIA) to measure body composition. In simple terms, it sends a safe, low-level electrical current through the body at multiple frequencies. The device measures the resistance to this current, called impedance, independently through each body segment. No dunking, no pinching, no discomfort. The child simply stands on the device and holds the hand electrodes for 60 seconds.
What the InBody H30 Measures: 20+ Parameters in 60 Seconds
The InBody H30 result sheet provides a comprehensive body composition profile across more than 20 parameters. Specifically, the most clinically significant outputs for youth health and immunity assessment include the following:
- Fat Mass (kg): Total body fat weight tracked against age- and gender-specific reference ranges for children and adolescents.
- Skeletal Muscle Mass (kg): Total lean muscle weight is a direct indicator of metabolic health, glucose disposal capacity, and immune reserve.
- Body Fat Percentage (%): The proportion of total body weight that is fat tissue assessed against pediatric norms, not adult reference ranges.
- Body Water Levels (litres): Total body water, intracellular water, and extracellular water providing the ECW/TBW ratio as an inflammation and nutritional status marker.
- Muscle-Fat Analysis: A visual comparison of the child’s muscle and fat levels relative to their height an immediately interpretable indicator of whether composition is balanced.
- Obesity Analysis: BMI and percent body fat assessed side by side allowing clinicians to identify thin-fat cases that BMI alone misses.
- Growth Graphs: Longitudinal charts of weight, height, BMI, and body composition parameters enabling growth trajectory monitoring across multiple visits.
- Weight Control Information: Target fat mass and muscle mass values giving parents and clinicians a specific, actionable goal rather than a vague “eat less, move more” instruction.
Body Composition Monitoring in the New Normal: Schools, Clinics, and Families
As schools and educational institutions return to full operation, they face a health challenge that did not exist before the pandemic: a cohort of students whose physical health deteriorated measurably during lockdown. Consequently, the standard annual height-and-weight check is no longer sufficient. What is needed, instead, is a systematic approach to body composition monitoring, one that identifies students at metabolic and immunological risk before clinical disease develops.
Integrating InBody H30 Into School Health Programmes
The InBody H30 is well-suited to school-based health programmes for several reasons. First, the scan takes under 60 seconds, making it practical to screen an entire class in a single session. Second, the result sheet is immediately interpretable by teachers, school nurses, and parents; it does not require specialist interpretation. Third, the growth charts enable year-on-year tracking, so schools can monitor whether student health is improving or deteriorating over time.
Furthermore, the personalised, visual nature of the InBody H30 result sheet motivates students and families to engage with health in a way that abstract BMI numbers do not. When a student can see exactly how much of their body weight is muscle versus fat and whether that balance is moving in the right direction, it creates genuine motivation for the dietary and physical activity changes that actually improve health.
Recommended Clinical Protocol for Adolescent Body Composition Monitoring
For clinicians working with children and adolescents, the following monitoring schedule is recommended based on current evidence and the capabilities of the InBody H30:
- Baseline scan at first clinical contact establishes the patient’s current body composition profile and flags any immediate risks (high fat mass, critically low muscle, elevated ECW/TBW ratio).
- A follow-up scan at 3 months assesses whether dietary and physical activity interventions are producing measurable body composition change.
- 6-monthly scans thereafter track development across the pubertal growth period, allowing early detection of unfavourable composition trajectories.
- An annual scan for healthy patients provides a routine developmental record and maintains engagement with health monitoring.
- Additional scan post-illness (including post-COVID recovery) detects muscle wasting and elevated ECW/TBW ratio, guiding nutritional rehabilitation.
POST-COVID RECOVERY NOTE
Children and adolescents recovering from COVID-19, including those who experienced mild illness, may show measurable decreases in skeletal muscle mass and elevations in the ECW/TBW ratio. These changes are not detectable by weight or BMI. An InBody H30 scan at the point of recovery provides the data needed to guide nutritional rehabilitation and monitor return to full physiological health. This is particularly relevant for students returning to physical education and competitive sport after COVID-19 illness.
Nutrition and Physical Activity: Building the Body Composition That Supports Immunity
Body composition does not change through awareness alone. It changes through specific, targeted interventions in nutrition and physical activity and it is only through body composition monitoring that clinicians and parents can confirm whether those interventions are working. Specifically, the following evidence-based recommendations apply to Indian children and adolescents seeking to improve body composition and immune readiness.
Protein: The Most Under-Consumed Nutrient in Indian Adolescent Diets
Research consistently shows that Indian adolescent diets are significantly deficient in protein, the macronutrient most directly responsible for building and maintaining skeletal muscle mass. Furthermore, this deficiency is particularly pronounced in vegetarian households, where high-quality complete protein sources are less frequently consumed. Consequently, even adolescents who appear well-nourished by caloric standards may be building fat mass at the expense of muscle mass, setting up the thin-fat phenotype from an early age.
The recommended protein intake for Indian adolescents is 0.8–1.2g of protein per kilogram of body weight per day. Good sources in the Indian diet include: dal and legumes, paneer, eggs, curd and buttermilk, nuts and seeds, and soy-based foods. Additionally, spreading protein intake across three or more meals rather than consuming most protein at a single meal has been shown to maximise muscle protein synthesis in growing bodies.
Exercise: Resistance Training Is Not Just for Adults
There is a persistent misconception that resistance training exercises designed to build and preserve muscle mass are inappropriate for children and adolescents. In reality, current evidence from pediatric sports medicine firmly contradicts this view. Age-appropriate resistance training, when properly supervised, is safe, effective, and beneficial for children from approximately age 8 onwards.
Specifically, a programme combining aerobic activity (30 minutes daily) with two to three sessions of bodyweight or resistance exercise per week has been shown to improve skeletal muscle mass, reduce fat mass, lower visceral fat levels, and improve insulin sensitivity in adolescents, all of which directly strengthen immune function. Moreover, the mental health benefits of regular physical activity, such as reduced anxiety, improved sleep, and better mood regulation, are particularly relevant for adolescents who experienced the social isolation and psychological stress of pandemic lockdowns.
Frequently Asked Questions
The InBody H30 uses a safe, low-level electrical current that is completely harmless and not felt by children. The scan takes under 60 seconds, requires no needles or radiation, and is suitable for most children except those with implanted pacemakers or defibrillators without medical clearance.
Children and adolescents usually experience milder COVID-19, but poor body composition (high fat and low muscle) increases the risk of inflammation, slower recovery, and weaker vaccine response.
A weighing scale only shows total body weight and cannot distinguish between fat, muscle, or body water. The InBody H30 analyses over 20 body composition parameters, helping clinicians and parents understand what a child’s weight is made of and how it impacts overall health.
BMI cannot distinguish fat from muscle, which is a major limitation, especially in India.
A child may have a “healthy” BMI yet still carry high body fat, low muscle mass, and elevated visceral fat risks that tools like the InBody H30 can detect in under 60 seconds, while BMI misses them.
The InBody H30 is available across pediatric clinics, school health programs, sports medicine facilities, and community wellness centres throughout India. For nearby scanning centres or institutional deployment in schools and corporate wellness programs, contact InBody India.
Key Takeaways: Youth Body Composition and COVID-19 Immunity
- Body composition, not weight or BMI, is the key determinant of immune function in children and adolescents. High fat mass suppresses immunity; low muscle mass reduces the amino acid reserves needed to sustain an immune response.
- Indian adolescents face a dual crisis: excess fat and insufficient muscle occurring simultaneously, the sarcopenic obesity pattern that standard BMI screening cannot detect.
- The pubertal window is critical. Body composition trajectories established during adolescence are among the strongest predictors of adult metabolic and immune health. Intervention during this period delivers lifelong benefit.
- The InBody H30 measures 20+ parameters in under 60 seconds, including paediatric-specific fat mass, skeletal muscle mass, body water distribution, growth charts, and obesity analysis, all calibrated for Asian-population reference values.
- Post-COVID recovery in children should include body composition monitoring to detect muscle wasting and elevated ECW/TBW ratio, and to guide targeted nutritional rehabilitation.
- Evidence-based intervention adequate protein (0.8–1.2g/kg/day), daily aerobic activity, and supervised resistance training improves body composition, strengthens immunity, and reduces long-term disease risk in Indian adolescents.
Know Your Child’s Body Composition. Protect Their Health Now and in the Future.
An InBody H30 scan takes under 60 seconds and gives clinicians, parents, and educators the body composition data needed to make genuinely informed decisions about a child’s health before disease develops, not after.

Find an InBody Scanner Near You
References & Further Reading
- International Diabetes Federation. IDF Diabetes Atlas, 10th Edition. Brussels: IDF, 2021.
- Yajnik CS, Yudkin JS. “The Y-Y paradox.” The Lancet. 2004;363(9403):163.
- Misra A, et al. “Consensus statement for diagnosis of obesity for Asian Indians.” JAPI. 2009.
- Asian Working Group for Sarcopenia. “2019 Consensus Update.” JAMDA. 2020.
- DeFronzo RA, et al. “Skeletal muscle insulin resistance is the primary defect in type 2 diabetes.” Diabetes Care. 2009.
- WHO Expert Consultation. “Appropriate body-mass index for Asian populations.” The Lancet. 2004;363(9403):157–163.
- World Health Organization. “Obesity and overweight — youth and adolescents.” WHO Fact Sheet. 2024.
- InBody Co. “Validation of InBody BIA against DEXA in diverse clinical populations.” InBody White Paper Series. Seoul: InBody Co., 2022.
